
Placenta previa occurs when the placenta blocks the cervix in pregnancy. During pregnancy, the placenta develops inside your uterus. It is an organ that resembles a sac that provides the fetus with nutrition and oxygen via the umbilical cord.
Throughout pregnancy, the placenta grows and expands. Early in pregnancy, it’s normal for it to be low in your uterus. The placenta should ascend to the top of your uterus throughout the third trimester, which spans weeks 28 through 40 of pregnancy. This takes place to give your baby an unobstructed route to the vagina for delivery. When the placenta does not ascend to the top of your uterus, it is known as Previa. It indicates that the placenta is obstructing your baby’s ability to leave your vagina.
Which placenta previa kinds exist?
Placenta previa has different forms. One form is when the placenta is at the edge of your cervix. This is called marginal placenta previa. It’s not covering your cervix; it’s just touching it. Before your baby’s due date, this kind of placenta previa is more likely to go away independently.
Partial placenta previa: Your cervix is partially covered by the placenta. Placenta previa, also known as complete or entire, is when the placenta covers your cervix and blocks your vagina. It is less common for placenta previa of this kind to heal on its own. Vaginal bleeding during pregnancy and labor can be caused by any kind of placenta previa. The majority of patients will need a Caesarean (C-section) delivery due to the increased risk of hemorrhage.
How Often Does Placenta Previa Occur?
Roughly 1 in 200 pregnancies result in placenta previa. Usually, during an ultrasound in the second trimester, pregnancy care providers make the diagnosis.
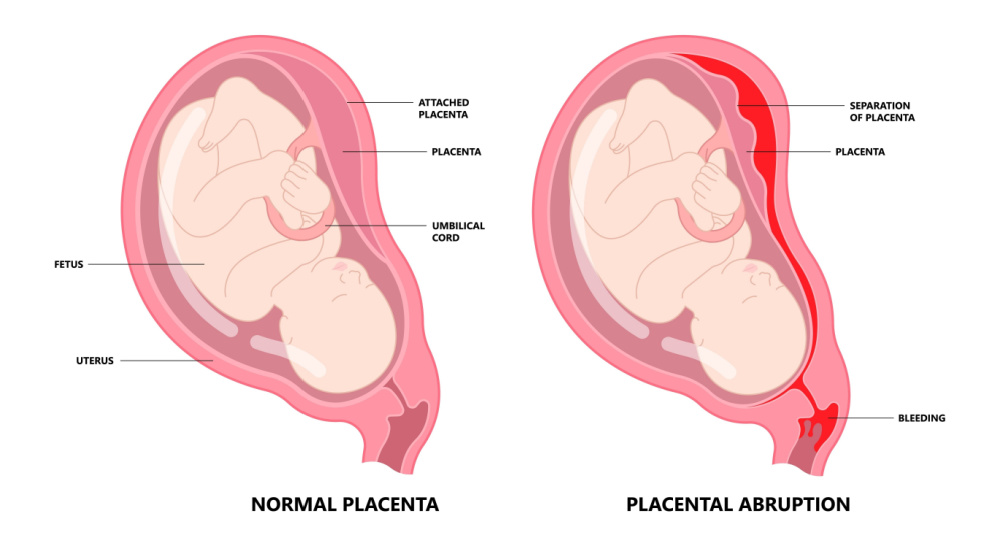
What distinguishes placental abruption from placenta previa? The placenta covers all or part of your cervix when you have placenta previa. The placenta remains linked to your uterus despite its complex position. When the placenta separates from your uterus, it is called a placental abruption. Vaginal bleeding can occur during both pregnancy and labor due to certain causes.
Does the placenta anterior and placenta previa interchange? Anterior placenta and placenta previa are two different things. In your uterus, the placenta can grow anywhere. The placenta is implanted in the front of your body if it is placed anteriorly. Consider the anterior placenta to be a cushion between your tummy and your unborn child.
Placenta Previa and Fibroids During Pregnancy
Obstetric hemorrhage is a major cause of maternal morbidity and mortality. Worldwide, it is responsible for placenta previa and fibroids during pregnancy. Placenta praevia can cause fatal bleeding in the third trimester. This condition contributes to twenty percent of episodes of bleeding before birth. Anomalous placenta implantation in the lower uterine segment defines it. The placenta covers the internal os, fully or partially. Five cases of placenta previa are reported for every 1,000 pregnancies. The figure rises to 12.2 per 1,000 pregnancies in Asian nations.
One of the possible risk factors for aberrant placental implantation is uterine fibroids. Research has shown that the presence of a fibroid uterus doubles the risk of placenta previa. This risk can increase two to three times. Pregnancy is not always associated with cervical fibroid, an unusual variation of uterine fibroid. They occasionally have a big impact on how a pregnancy develops and turns out. There are several known problems [1]. These include infection, retention of urine, premature labor [2], obstructed labor [3], and an increased risk of hemorrhage [4]. The risk is six times more [5]. The exact role that cervical fibroids play in the formation of placenta previa is yet unknown. Nonetheless, obstetricians must navigate a difficult situation during pregnancy. This occurs when a cervical fibroid complicates placenta previa.
A Case Study
A 27-year-old lady with abdominal pain and vaginal bleeding was admitted to the labor room at 37 weeks and 2 days of gestation. She had no living issues and was a second gravida. She gave birth to twins vaginally prematurely at 36 weeks gestation a year and a half ago, and both kids died at birth.
In the current pregnancy, a 20-week ultrasound showed a cervical myoma. The myoma measured 11.5 cm by 8.5 cm. The placenta was on the right side of the uterus. The patient did not receive routine prenatal care. Other related comorbidities did not exist for her.
She appeared pale upon general inspection, but her vital signs remained steady. During the obstetrical examination, the uterus was found to be of term size. The uterus showed mild contractions and moderate vaginal bleeding. Following an ultrasound scan, a central placenta previa and a central cervical fibroid measuring 10 cm by 8 cm were discovered. The estimated weight of the fetus, which had a cephalic presentation, was 3.1 kg. There was a sufficient amount of amniotic fluid. During the blood examinations, they found anemia with a hemoglobin percentage of 7.8 gm%. Abnormal liver enzymes were also found, which suggested maternal cholestasis.
The results of the remaining blood tests were within normal bounds. She had an antepartum hemorrhage and central placenta praevia. An emergency cesarean surgery was scheduled for her. Before surgery, blood components were cross-matched. The informed agreement was acquired, considering the possibility of a cesarean hysterectomy in the event of uncontrollable intraoperative hemorrhage. Using a Pfannenstiel incision, the abdomen was made accessible during the procedure. First, the peritoneal uterovesical fold was separated. Next, a careful incision was made in the lower segment above the fibroid. By slicing through the placenta, a live, term baby was delivered. With an APGAR (Appearance, Pulse, Grimace, Activity, and Respiration) score of 9/10, the baby cried from the moment of birth. It was easy to remove the membranes from the placenta. There was a central cervical fibroid that was extending posterolaterally and measured about 10 cm by 8 cm. The doctors used special stitches to stop the heavy bleeding. The stitches were placed where the placenta separates from the uterus. Both arteries in the uterus were clamped.
Furthermore, uterine tamponade was performed with two 50 mL Foley catheter bulbs. Bleeding was managed and uterotonics were administered. Two layers of closure surrounded the uterus. The abdomen was closed in layers and a pelvic drain was installed. During surgery, two red blood cells were transfused. The patient was then monitored in the high-dependency unit. The remainder of the postoperative period went without incident. The patient was released on the fifth postoperative day. Instructions were given to monitor the cervical fibroid over six weeks. This was during the postpartum period. Discussion: It is rare for uterine fibroids to coexist with pregnancy. 1.6% to 10.7% is the reported prevalence range. Less than 1% of all fibroids reported during pregnancy are cervical fibroids, making them the rarest form. There is very little literature on cervical fibroids during pregnancy other than case reports and case series. They typically do not show symptoms, but sometimes do affect pregnancy outcomes. Research has shown that pregnant women with fibroid uteri have a higher chance of developing placenta previa.
According to one study, there is a 3.53-fold increase in the incidence of placenta previa in cases of uterine leiomyoma measuring 5 cm or more. The varieties of fibroid that are usually involved in improper placentation are not mentioned, though. Furthermore, it is unknown if aberrant placental implantation is related to cervical fibroids in any way. During pregnancy, there is only one case study of numerous cervical fibroids that complicate placenta previa. The combination of placenta previa and cervical fibroid presents a problem for obstetricians. Both conditions can cause life-threatening complications during childbirth.
Cervical fibroids can cause problems during pregnancy like fibroid degeneration. Postpartum hemorrhage and premature labor are other potential issues. Pressure from the fibroids can also lead to urinary retention. Furthermore, the risk of complications is doubled when placenta praevia and cervical fibroid coexist. During the peripartum phase, massive bleeding is the most terrifying potentially fatal consequence. Tertiary care hospitals are the best places to handle these cases. They are equipped with multidisciplinary teams, critical care units, and 24-hour access to blood supplies. It is nearly impossible to have a vaginal delivery in this instance. This is especially true in cases of central placenta praevia. Therefore, the best course of action is to have an operation. The cervical fibroid on the incision line makes lower-segment cesarean sections difficult. Lower-segment cesarean sections might cause profuse bleeding if the fibroid is accidentally cut.
In addition, if the placenta praevia is anterior, the only way to deliver the fetus is by cutting through the placenta, which worsens the bleeding. Blood products should be ready for the operating team to stop the severe bleeding. The use of medical and conservative approaches to stop bleeding should be done gradually. Uterotonics help control bleeding. Additional techniques include iliac artery ligation, embolization, balloon tamponade, and uterine artery ligation. Cesarean hysterectomy is the first line of treatment for morbidly adherent placenta. It is used when conservative measures fail. In preparation for a hysterectomy, the surgical team needs to get ready early. The patient needs close monitoring in a high-dependency unit after surgery. This is because they may require a large blood transfusion and may experience related problems. Having a myomectomy during a cesarean has a high risk of failure. This is due to the chance of a hysterectomy and hemorrhagic complications.
Few obstetricians would venture to remove a fibroid when it is linked to placenta previa. However, reports on myomectomy after C-section show no major side effects. In most cases, fibroid therapy during cesarean section requires caution. This is especially true if it’s associated with placenta previa. A myomectomy, hysterectomy, or uterine artery embolization may be considered. This depends on the patient’s desired fertility, mass location, and symptoms. The patient who came in for treatment was in active labor and had an antepartum hemorrhage. A previous ultrasound report of the patient revealed a big cervical fibroid. Our center’s ultrasonography found a central cervical fibroid. It also discovered placenta praevia. Both conditions required an emergency cesarean procedure. We braced ourselves for the huge hemorrhage that we expected after giving birth. The procedure stretched the lower uterine segment to create an incision. The incision was made above the cervical fibroid. The placenta was then separated to deliver the baby. There was expected bleeding. It was treated with various methods like ligation and sutures. Uterotonics were also used. We would have had to consider two options if the bleeding didn’t stop. Hysterectomy or internal artery ligation.
Conclusion
Obstetricians struggle to handle a large cervical fibroid with central placenta praevia. This condition often causes antepartum hemorrhage. Thoroughly assess to save the lives of the mother and fetus. Sufficiently plan for unforeseen issues and quickly intervene. Preoperative ultrasound is crucial for locating the fibroid near the placenta and cervix. Before the cesarean section, it is done to determine the incision. The incision is in the lower uterine segment. Ideally, the incision line should not cross the cervical fibroid. This helps avoid significant blood loss. Whenever possible, myomectomy during cesarean section should be avoided. Massive postpartum hemorrhage is known to be caused by placenta praevia. During deliveries, it is important to use obstetric settings. These settings should have blood banks, qualified medical professionals, and critical care services. Using uterotonics, postpartum hemorrhage can be effectively treated. If medication fails, implement conservative measures like uterine tamponade. Use hemostatic sutures and step-by-step devascularization operations as well. Interventional radiological techniques can stop bleeding when facilities are available. If conservative measures fail, a hysterectomy should be considered. It can be a life-saving intervention.
Disclaimer: “HealthLink.news does not have any intention to provide specific medical advice, but rather to provide its users and the general public with information to understand their health better. All content (including text, graphics, images, information, etc.) provided herein is for general informational purposes only and is not a substitute for professional medical advice, care, diagnosis, or treatment. HealthLink.news makes no representation and assumes no responsibility/ liability for the accuracy of the information, advice, diagnosis, or treatment provided herein or on its website. NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY IN SEEKING TREATMENT BECAUSE OF SOMETHING YOU HAVE READ HERE OR ACCESSED THROUGH THE HealthLink.news WEBSITE.”
